Introduction to Milialar Understanding
Milialar means very tiny, unimportant, white or yellowish lumps on the skin. Since the cysts lack openings or openings, unlike pimples, they are immune to conventional crushing or popping. These emerge as a result of cellular debris becoming entrapped beneath the outermost layer of the skin.
Knowing the Symptoms and Signs of Miliaryar

Differences in size and color:
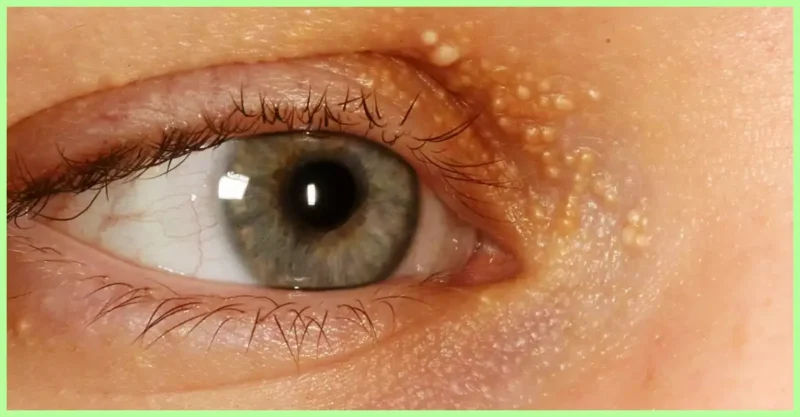
Milialar often have a white or yellow tone, are around the size of an average pinhead, and resemble tiny beads or seeds. These variations in size and color are common.
Common Body Sites:
Although milia can appear everywhere on the body, they are most frequently found on the face of a person, particularly close to the facial features and eyebrows. On rare cases, they are also seen on the tip of a person’s nose, top of the thorax, and the temples.
Risks of similar issues
Although medical operations are frequently fast and secure, they could have an aesthetic impact. The visibility of them may increase under specific conditions, such as exposure to strong sunlight, leading to aesthetic issues.
Militarization can happen for a variety of reasons, including
Keratin excess production and protein trapping: Excessive keratin, a skin proteins, can get buried under the layer of skin and cause milia.
Damage to the oil gland or sweat duct: Skin trauma, such as cuts or exposure to the direct sunlight, can injure the cells that generate moisture from the ducts, hastening the milia growth procedure.
Cosmetics and skincare items: Certain health and cosmetic items, particularly heavy and improper moisturizers, might clog pores and result in milia.
Medical diagnosis and evaluation

Milia is frequently identified by dermatological or other specialized healthcare providers. Doctors thoroughly examine the cysts visually, noting their size, design, and colour. Sometimes magnification tools like dermatologist are used for a more complete examination. A complete assessment considers someone’s medical history, prescription drug use, and hygiene routine. Often a microscopic examination or dissecting of a piece of a single of the cysts’ contents is required for a clear diagnosis.
Different Milia
Based on their main reasons, milia are divided into numerous types:
First Milia: These are among the most prevalent and afflict people of every age group. They appear when dead cells from the skin clog sweat ducts.
Additional Milia: They may appear after some skin procedures like the procedure or laser resurfacing, as well as after skin traumas or injuries like burning or blisters.
Newborn Milia: Newborns are affected by this widespread disorder soon after birth. The cysts are benign and usually go away on their very own in a few weeks.
Plaque Milia: A group of cysts surrounding an inflamed, raised region of skin characterizes this uncommon kind of milia.
Various Milia
Milia are categorized into various categories according to their primary causes:
Initial Milia: These are amongst the most common conditions, affecting people of all ages. When sweat ducts become blocked by cellular debris, they develop.
A second Milia: This may develop following particular skin operations, such as laser rejuvenation or the process, as well as following skin trauma or injury, such as acute scorching or blisters.
Infant Milia: This common condition affects infants shortly after birth. The innocuous cysts typically disappear on their own within a couple of weeks.
Mural Milia: This unusual kind of milia is characterized by a cluster of cysts encircling an inflammatory, elevated patch of skin.
Milia Treatment Options
Milia treatment is based on the determination, size, and location of the lesions. Typical forms of treatment include:
Automatic Resolution: Milia frequently disappears on their own without special care.
Cosmetic dermatology procedures: Cryotherapy, laser treatments, peels with chemicals, and exfoliation are a few of the methods doctors use to eradicate milia.
Use of Topical Retinoids: Topical retinoids available both on medication and free of charge, may occasionally aid in the removal of milia.
Home Treatments: Miliaria can be treated at home with gentle scrub and the right skincare regimens.
Prevention Techniques and Do-It-Yourself Fixes

Natural remedies and precautions include:
- Using lotion or wearing appropriate attire in order to safeguard skin from the sun.
- Milia can appear less noticeable when taken with over-the-counter medications including benzoyl peroxide, acidic substances (also known as vitriolic acid), or lactic acid.
- In severe situations, doctors could use an intravenous antibiotic like metronidazole or penicillin.
Conclusion
Milia are usually not harmful, but for some people, their appearance can be an issue. This thorough overview covers their causes, remedies, and mitigation strategies. It emphasizes the significance of expert assessment and direction for accurate identification and customized milia treatments. At every age, milia can be prevented and managed by following proper skincare habits and using the right protection.
FAQ:
A phrase that sounds like a misprint is military. This could be referring to “milia,” which are very small, harmless skin cysts.
Milia is mostly only an aesthetic concern; it very rarely causes pain.
Because milia lack an opening, it is not advisable to crush them; doing so could irritate the skin and increase the risk of infection.
Milia may go away on one’s own without the need for treatment. Yet they might persist for a long time in rare circumstances.
Dermatological methods, topical retinoids that are natural treatments, or waiting for milia to go away spontaneously are all possible forms of treatment.
Milia can be treated at home with mild exfoliating and correct skincare regimens, but it is advised to see a medical professional for an accurate diagnosis.
Excessive keratin manufacture, injury to sweat or oil glands due to the usage of specific cosmetics or skincare items, and hereditary susceptibility are a few causes of milia.
Yes, there are different forms of milia, including the following: primary, secondary, neonatal, and bumps on a plate.